Available Products: Pharmaceuticals¶
Child date of birth: 08/04/2021. Age at time of this review: ~4 years 11 months.
This document lists the household pharmaceutical and cosmetic products relevant to the child's eczema management, including day-to-day products and a small number of episodic prescription medicines that materially affect flare interpretation (such as oral antibiotics). Products are categorised, annotated with their role, and a treatment plan is provided below.
A. Emollients and barrier moisturisers¶
These are the foundation of daily care. Used every day, between flares and during flares. No prescription required.
| Product | Key ingredients | Role | Notes |
|---|---|---|---|
| LA ROCHE-POSAY LIPIKAR BAUME AP+M | Shea butter, niacinamide, microbiome-rebalancing complex | Primary leave-on emollient | Thick baume; excellent for whole-body application after bathing; suitable for atopic skin |
| BIODERMA ATODERM INTENSIVE BAUME | Glycerol, niacinamide, microbiome complex | Primary leave-on emollient (alternative / rotation) | Thick baume; specifically formulated for atopic skin; can alternate with Lipikar |
| AVENE XERACALM A.D. creme | I-modulia (microbiome), ceramides, Avène Thermal Spring Water | Secondary emollient (lighter texture) | Lighter than the baumes above; better for less severe days or face application |
| BEPANTHENE ECZEMA emollient cream | Dexpanthenol 1% (provitamin B5), glycerin, emollient base (petrolatum, liquid paraffin) | Barrier-repair emollient for atopic skin | Dexpanthenol supports keratinocyte regeneration and has mild anti-inflammatory action; suitable from birth; no fragrance, no preservatives in most formulations; useful on face, folds, and recovering skin; distinct from regular Bepanthene/Bepanthen 5% cream (that is for wounds and nappy rash — different concentration and purpose) |
Usage guidance for Bepanthene Eczema: - Use as a leave-on emollient (not wound cream): apply to whole body or targeted dry/recovering areas after bathing - Apply before TCS (emollient first, then TCS on affected patches after a few minutes, or vice versa — both approaches are used; the important thing is not to dilute the steroid by applying emollient immediately on top) - Dexpanthenol has evidence from small RCTs (e.g., Ebner et al., Pediatr Dermatol, 2002) supporting improved SCORAD and barrier function in mild-to-moderate AD - Suitable for the child's face, eyelids, and skin folds where the heavier baumes may feel occlusive - Can be alternated with Lipikar/Atoderm on days when the heavier product is not tolerated or when skin is in recovery phase (State 4) - Do not confuse with Bepanthene wound–healing cream (5% dexpanthenol): that product is intended for nappy rash, abrasions, and wound healing — it is not equivalent to the Eczema formulation and is not optimised as a daily AD emollient
Recommendation: Lipikar Baume AP+M or Atoderm Intensive Baume as the daily default (thick, protective). XeraCalm A.D. cream or Bepanthene Eczema for face, folds, or recovering skin. Apply within minutes after bathing ("soak and seal").
B. Cleansers (rinse-off)¶
Used during bathing to replace soap. Do not leave on skin. No prescription required.
| Product | Key ingredients | Role | Notes |
|---|---|---|---|
| LA ROCHE-POSAY LIPIKAR SYNDET AP+ body wash | Niacinamide, shea butter, syndet base | Primary daily cleanser | Recommended first choice; syndet formula maintains skin pH; fragrance-free |
| A-DERMA EXOMEGA CONTROL gel lavant emollient | Rhealba oat extract, ceramides | Alternative cleanser / rotation | Gentle rinse-off emollient cleanser; can alternate with Lipikar Syndet |
Recommendation: Use one of these two for every bath or shower. Do not use regular soaps or foamy products. Duration: 5–10 minutes, lukewarm water.
C. Topical corticosteroids (TCS)¶
Prescription required. Anti-inflammatory treatment for active flares. Do not use without a clinician's guidance on duration and areas.
| Product | Active ingredient | Potency class | Area of use | Notes |
|---|---|---|---|---|
| Anticort | Hydrocortisone acetate 1% | Mild (Class I) | Face, neck, skin folds, scattered mild body flares | Safest option for face; first choice for sensitive areas and young children; mild enough for short-term repeated courses |
| Advantan | Methylprednisolone aceponate 0.1% | Potent (Class III) | Body flares only — trunk, limbs; NOT face | Once-daily application; limited to short courses (typically ≤14 days per site); do not use on face or thin skin |
Treatment plan role: - Use Anticort for face, neck, and folds - Use Advantan for body flares where Anticort is insufficient - Once a flare is controlled, consider proactive maintenance: apply Anticort to previously affected sites 2–3 times per week to prevent recurrence (discuss protocol with clinician — supported by Schmitt et al., Br J Dermatol, 2011)
Gap: No calcineurin inhibitor (tacrolimus/pimecrolimus) available — see Recommendations below.
D. Topical antibiotic¶
Prescription required. For visibly infected eczema (impetiginized lesions with honey-coloured crusting, pustules, or weeping).
| Product | Active ingredient | Role | Notes |
|---|---|---|---|
| Bactroban cream | Mupirocin 2% | Topical antibiotic for infected eczema patches | Apply to affected areas 2–3x daily for 5–7 days; do not use for more than 10 days; do not use prophylactically |
| Bactroban nasal ointment | Mupirocin 2% | Nasal Staphylococcus aureus decolonization | Only relevant if part of an explicit decolonization protocol (e.g., recurrently impetiginized eczema); not for routine use in the child |
| Xylanal gel | Amikacin sulfate 5% (50 mg/g as amikacin; 66.75 mg/g as amikacin sulfate) | Topical aminoglycoside antibiotic for infected skin | Aminoglycosides cover gram-positive and gram-negative organisms; amikacin's resistance profile complements mupirocin (different class). Contains methylparaben and propylparaben (E218/E216) — potential contact sensitizers in eczema skin; note and discontinue if irritation or worsening occurs. Apply to infected areas as prescribed. |
Important: Both Bactroban and Xylanal are for infected skin only. Routine or prophylactic use drives resistance. They are complementary, not interchangeable — mupirocin (Bactroban) remains the first-line choice for impetiginized eczema; Xylanal can serve as an alternative when mupirocin is not available or where resistance is suspected. Bactroban nasal is for nasal decolonization protocols, typically of a caregiver rather than the child, unless specifically prescribed.
E. Oral / systemic antibiotics (episodic prescription use, not routine eczema treatment)¶
These medicines matter because they may have been prescribed during periods when eczema looked infected or when another childhood infection happened at the same time. They are not standing eczema medicines and should not be restarted without medical advice.
| Product | Active ingredient | Usual role | Relevance to eczema | Key cautions |
|---|---|---|---|---|
| Ceclor | Cefaclor | Oral second-generation cephalosporin antibiotic | The official leaflet includes skin and soft tissue infections, so this is a plausible oral option when a clinician thinks the eczema infection is bacterial and needs systemic treatment. It is not the standard first-choice oral antibiotic in NICE for infected eczema, so it should be treated as episode-specific rather than as a routine eczema medicine. | Reported side effects include diarrhoea, nausea, vomiting, rash, itching, and urticaria. |
| Amoxil | Amoxicillin | Oral aminopenicillin antibiotic | More commonly used for ear, throat, sinus, chest, urinary, or dental infections than for infected eczema. Official susceptibility guidance states that most Staphylococcus aureus are resistant to amoxicillin because they produce penicillinase, so it is not a strong empiric choice for classic impetiginized eczema alone. | Common adverse reactions include diarrhoea, nausea, and skin rash. If used during an eczema period, record whether it was actually prescribed for the skin or for another infection happening at the same time. |
| Augmentin | Amoxicillin + clavulanic acid | Broader oral beta-lactam / beta-lactamase inhibitor antibiotic | The official label includes skin and soft tissue infections, making it more plausible than amoxicillin alone when a clinician wants oral treatment for cellulitis, more extensive infected eczema, or broader bacterial coverage. It is still broader-spectrum than the simple first-choice oral regimens highlighted by NICE for routine infected eczema. | Common adverse reactions are diarrhoea, nausea, and vomiting; candidiasis and rash can also occur. GI upset may be reduced by taking it with a meal. |
How to think about oral antibiotics in eczema: - NICE says do not routinely offer either a topical or oral antibiotic for secondary bacterial infection of eczema in children who are not systemically unwell - If an antibiotic is used, a topical antibiotic is usually more appropriate for localised, non-severe infection, while an oral antibiotic is more appropriate when infection is widespread or severe - If the child is systemically unwell, NICE says to offer an oral antibiotic - Even when antibiotics are given, continue emollients and topical corticosteroids for the underlying eczema unless a clinician advises otherwise
Practical recommendation for this child: The main value of adding Ceclor, Amoxil, and Augmentin to the treatment map is not to self-select among them at home. It is to interpret the history correctly. Each time one is used, record:
- what infection the doctor was treating (eczema/skin, ear, throat, chest, sinus, other)
- whether the skin improved clearly, partly, or not at all
- whether there were GI side effects, rash, thrush/candidiasis, or behaviour/appetite changes
Source note: Eczema-specific prescribing principles above are from NICE NG190 on secondary bacterial infection of eczema (recommendations 1.1.5 to 1.1.7 and 1.1.13). Product-level facts come from official medicine documents for Cefaclor oral suspension, Augmentin suspension, and Amoxicillin.
F. Antiseptic wash (microbial decolonization)¶
| Product | Active ingredient | Role | Notes |
|---|---|---|---|
| OCTENISAN wash lotion | Octenidine dihydrochloride | Antiseptic whole-body wash for Staph aureus decolonization | Use as bath wash substitute during or around flares driven by skin colonization; lathers like a wash; leaves antimicrobial residue; do not rinse off immediately; suitable for infants and children |
Recommendation: Use Octenisan in place of the regular cleanser during phases of suspected bacterial colonization or during flares with infected appearance. Not for daily permanent use — reserve for 1–2 week courses during active or prone periods, then return to emollient cleansers. Follow with emollient as usual.
G. Skin repair and wound care¶
| Product | Key ingredients | Role | Notes |
|---|---|---|---|
| BIODERMA Cicabio Creme | Sucralfate, zinc oxide, antibacterial complex | Skin repair for damaged, fissured, post-flare skin | Promotes healing of excoriated or cracked areas; mild antibacterial action; useful during the recovery phase after a flare |
| Betadine antiseptic solution | Povidone-iodine 10% | Spot wound antisepsis only | NOT for eczema skin. Povidone-iodine is cytotoxic to healing skin cells and should not be applied to eczema patches or broad areas; reserve only for isolated contaminated wounds |
| MeliMpampa Κεραλοιφή Σώματος Επουλωτική με Σπαθόχορτο & Πρόπολη 40 ml | Hypericum perforatum (St. John's Wort) extract, propolis (bee resin), beeswax base | Natural healing ointment — restricted use | Use with caution. Propolis is a known contact allergen on atopic/compromised skin. Only for recovery-phase (State 4) skin if at all — see notes below. |
Recommendation: Use Cicabio on fissured or excoriated areas during healing. Keep Betadine for isolated wound cleaning only — never apply to eczema rash or active skin patches.
Usage guidance for MeliMpampa Healing Ointment (Κεραλοιφή με Σπαθόχορτο & Πρόπολη):
Ingredients and proposed mechanism:
- Hypericum perforatum (St. John's Wort / Σπαθόχορτο): The active constituent is hyperforin (anti-inflammatory, mild antibacterial). One small double-blind RCT (n=18 completers; Schempp et al., Eur J Dermatol, 2003 — PMID 12807340) compared a cream standardised to 1.5% hyperforin against vehicle in mild-to-moderate AD. Hyperforin cream was significantly superior on a modified SCORAD at all visits (days 7, 14, 28; p < 0.05), with a non-significant trend toward reduced Staphylococcus aureus colonization and good skin tolerance. This is a single small trial — no replication against TCS or calcineurin inhibitors exists. The MeliMpampa product is not standardised to a declared hyperforin content, so clinical equivalence to the trial preparation cannot be assumed.
- Propolis: A complex bee resin containing flavonoids (chrysin, kaempferol, pinocembrin) and caffeic acid derivatives that inhibit mast-cell activation and allergic mediators in preclinical models (Liew et al., Front Pharmacol, 2022 — PMID 35126124). However, propolis is a well-documented contact allergen, particularly when applied to inflamed or atopic skin (de Groot, 2013 — PMID 24201459; Mezei et al., 2022 — PMID 36153726). Risk of sensitization is elevated in atopic dermatitis because the impaired skin barrier increases allergen penetration.
When it could be considered (if at all):
- Only during Phase 4 (recovery / healing) — dry, fading, non-inflamed, non-infected skin
- Spot application to intact or near-intact healing areas only; NOT to active flare patches, open excoriations, or infected areas
- Monitor closely: new redness, new itching, or new rash after application suggests contact sensitization — stop immediately
When to avoid entirely:
- Active eczema flare (State 2) — propolis can worsen inflamed skin
- Infected or colonized skin (State 3) — occlusive beeswax base can trap bacteria
- Open excoriations, scratch wounds, or weeping skin — broken barrier increases sensitization risk
Overall assessment for this child: This is a natural / complementary product with some biological plausibility (hyperforin data) but a meaningful safety concern (propolis contact allergy on atopic skin). It is not a recommended eczema treatment in NICE, EuroGuiDerm, or AAD guidelines. If trialled, use only on clearly recovered non-inflamed skin, test a small area first, and stop at the first sign of a new reaction. Do not substitute for Cicabio, emollients, or TCS.
H. Oral antihistamine (adjunct only, not core eczema treatment)¶
| Product | Active ingredient | Role | Notes |
|---|---|---|---|
| Xozal oral solution | Levocetirizine 0.5 mg/ml | Non-sedating oral antihistamine that may sometimes help with itch when there is an allergic or urticaria-like component | Not a primary eczema treatment. Main licensed uses are allergic rhinitis and urticaria. For children aged 2 to 6 years, the official oral-solution leaflet gives a usual dose of 2.5 ml twice daily. Can be taken with or without food. Common side effects include sleepiness/drowsiness, tiredness, dry mouth, and headache. Even though it is a second-generation antihistamine, it can still make some children sleepy. |
How to think about Xozal in eczema: - Do not treat it as a replacement for emollients, topical steroids, or infection treatment - NICE says oral antihistamines should not be used routinely for atopic eczema in children - A non-sedating antihistamine may be considered when eczema is severe, itch is severe, or there is an urticaria/hives-like element - If sleep disturbance is the main problem during an acute flare, NICE instead discusses a short 7- to 14-day trial of an age-appropriate sedating antihistamine
Practical recommendation: Keep Xozal as an optional adjunct to discuss or use only within a clinician-agreed plan, especially if itching is severe, sleep is being disrupted, or the rash has an allergic / hive-like component. If it clearly causes sedation, behavioural change, or no meaningful benefit, it is probably not worth using for eczema symptoms alone.
Source note: Dosing and side-effect details above are from the official levocetirizine oral-solution patient leaflet (Xyzal / Greece: Xozal). Eczema-use framing is based on the NICE guideline on atopic eczema in under 12s (CG57 recommendations 1.5.1.33 to 1.5.1.35).
Recognising the skin state — which phase applies?¶
The hardest practical decision is telling eczema inflammation apart from infection, or deciding whether skin is in a quiet, active, or recovering state. The wrong call means either under-treating a flare or applying antibiotics where they are not needed (driving resistance). Use the table below and the linked photo references before deciding.
Quick decision guide¶
Is the skin red, itchy, and dry but WITHOUT crusts or oozing?
→ Phase 2 (active flare, no infection)
Is there yellow/honey crusting, pus, clear fluid weeping, or a bad smell?
→ Phase 3 (infected / heavy Staph colonization)
Did the child recently have a cold sore or herpes contact,
and is there a cluster of small punched-out blisters or erosions?
→ URGENT — see When to Get Help (possible eczema herpeticum — do not apply TCS)
Is the skin calm, dry, faintly pink in old flare sites?
→ Phase 1 (maintenance) or Phase 4 (recovery)
State-by-state recognition guide¶
State 1 — Baseline / quiet eczema¶
Maps to: Phase 1 (daily maintenance)
What you see: - Dry, slightly rough texture — like fine sandpaper - Faint pink or grey-brown tone in previously affected areas (post-inflammatory pigment change) - No active redness; no weeping; no crusts - Child may still itch mildly, especially at night or after sweating
What you feel: - Skin feels tight or slightly thickened in chronic areas (flexures, wrists, ankles) - May peel finely when scratched
What you do NOT see: - No bright red or hot patches - No fluid, pus, or crust - No papules (raised tiny bumps)
Photo reference:
DermNet NZ — Atopic dermatitis overview (dry / subacute presentations)
Representative image — quiet/baseline eczema (dry, slightly rough arm skin in a 5-year-old):
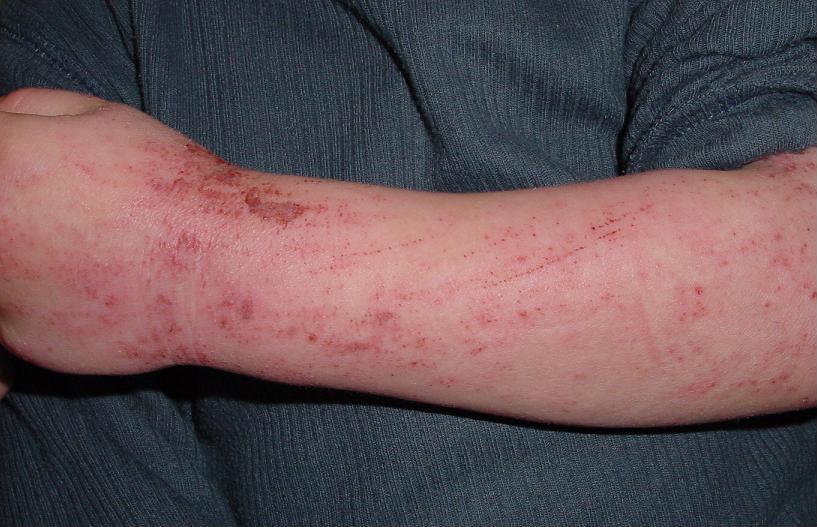
Eisfelder, CC BY-SA 3.0, via Wikimedia Commons — source¶
State 2 — Active eczema flare (no infection)¶
Maps to: Phase 2 (TCS + intensified emollient)
What you see: - Bright red or dark red patches — clearly more inflamed than baseline - Papules: small raised red bumps on the surface of the patch - Excoriations: scratch marks — linear red lines, sometimes with tiny scabs where nails broke the skin - Oedema (slight puffiness) in severe patches, especially eyelids or face - Lichenification in chronic sites: the skin looks thickened and leathery with exaggerated cross-hatching — sign of long-standing frequent flares
What you feel: - Warm to the touch compared with surrounding skin - Rough and slightly swollen
Child behaviour: - Active scratching, especially during transitions (waking up, coming in from outside, after bathing) - Rubbing face on pillow, carpet, or clothing - Sleep disruption
What you do NOT see: - No honey-coloured crust (a crust from scratch-and-dry is whitish-grey, not yellow) - No clearly defined pus - No strong smell
Key distinction from infection:
An eczema flare looks uniformly red and inflamed. Infected patches have a different texture — they look wet, crusty, or have a yellowish surface deposit. If in doubt, look for honey-coloured (not white/grey) crust and smell.
Photo references:
DermNet NZ — Atopic eczema, acute phase
DermNet NZ — Lichenification / lichen simplex
AAD — Eczema photo gallery
Clinical features diagram — erythema, papules, excoriations, lichenification:
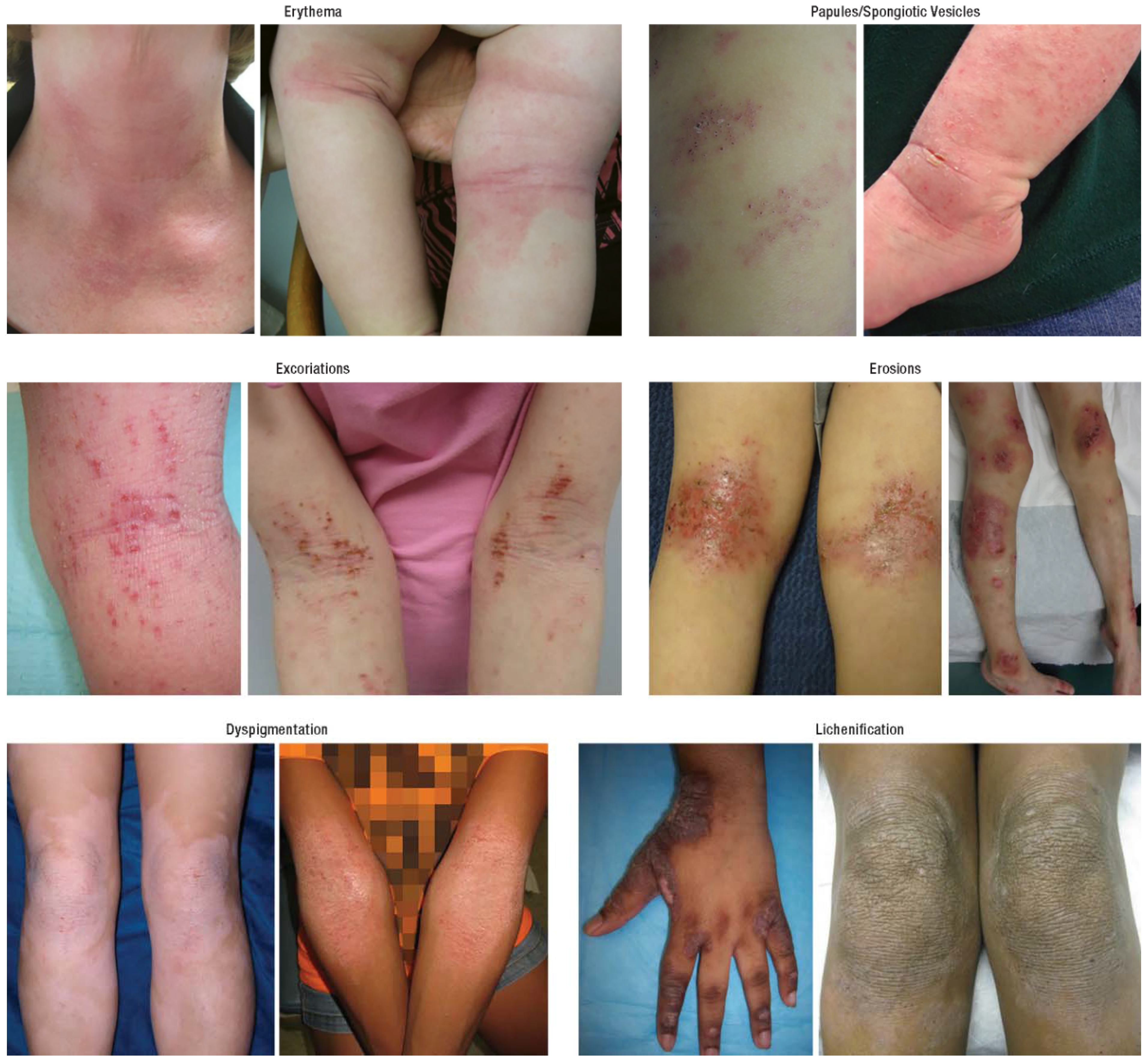
Siegfried EC, Hebert AA — J Clin Med 2015, CC BY 4.0 — source
State 3A — Infected eczema (impetiginization / Staph aureus)¶
Maps to: Phase 3 (Octenisan + Bactroban + continue TCS)
What you see: - Honey-coloured or golden-yellow crust — the single most reliable sign; crust is stuck, not easily lifted, and has a slightly waxy or varnished look - Weeping or oozing: the skin surface is wet, seeping clear or slightly cloudy fluid - Pustules: tiny pus-filled spots within or at the edge of the eczema patch - Crust forms after the pustule or ooze dries — can be patchy or sheet-like - Surrounding redness that extends slightly beyond the usual eczema boundary
What you smell: - A noticeable skin smell — sometimes described as "sweet" or "sour" — distinct from the usual dry-skin smell of eczema
Child behaviour: - Sudden marked worsening after a period of stability - More distress and scratching than a typical flare - May or may not have fever (fever is not required for skin infection)
Key distinctions: - White or grey crust = dried skin or scratch scab — not infected - Yellow/honey crust = infected until proven otherwise - If the eczema was controlled and suddenly gets much worse → think infection
Photo references:
National Eczema Association — Health conditions related to eczema
DermNet NZ — Impetigo (same organism, similar appearance)
National Eczema Society — Skin infections and eczema
State 3B — Eczema herpeticum (URGENT — do not apply TCS, seek urgent care)¶
Does NOT map to any home treatment phase — this requires medical assessment
What you see: - Clusters of small, round, uniform blisters (vesicles) — punched-out look, often described as "cookie-cutter" erosions - Blisters may be clear at first, then become cloudy or haemorrhagic (blood-tinged) - Rapidly spreading over hours — may involve face, neck, and body - Erosions where blisters have broken — raw, tender, shallow round pits - May appear in the child's existing eczema areas or around the mouth/eyes
Associated signs: - Fever, irritability, appearing generally unwell - Swollen lymph nodes near the affected area - Pain — often more pain than itch
Risk context:
Higher risk when the child has recently been in contact with an adult with an active cold sore (HSV-1), or after a chickenpox exposure (VZV). Children with severe eczema and elevated IgE are more susceptible.
What to do:
Stop all TCS immediately. Contact your clinician or go to A&E/emergency. This is a medical emergency in young children. Antiviral treatment (aciclovir) is required.
Photo references:
DermNet NZ — Eczema herpeticum
NHS — Atopic eczema
Representative image — eczema herpeticum (punched-out vesicles / erosions):
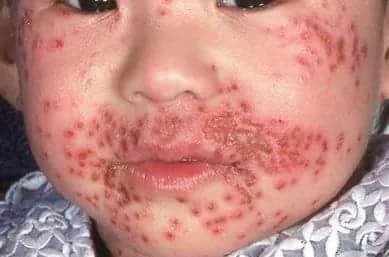
Mohammad2018, CC BY-SA 4.0, via Wikimedia Commons — source
Note the clustered punched-out erosions — different in texture and pattern from both plain eczema and impetigo.
State 4 — Recovery / healing after a flare¶
Maps to: Phase 4 (Cicabio on damaged areas + return to routine emollient)
What you see: - Redness is fading — the patch is turning from bright red to dusky pink or brownish-pink - Surface is dry and flaking (desquamation): the skin peels in fine sheets as it repairs - Fissures or small cracks visible on thicker areas (fingertips, heels, knuckles) — these can sting but are signs of healing, not new infection - Post-inflammatory hyperpigmentation: brown or grey patches where the flare was — common in darker skin tones; may persist for weeks
Child behaviour: - Less active scratching - Better sleep - Skin surface no longer hot to touch
What you do NOT see: - No new weeping or ooze - No honey crusting - No active papules
Key distinction from State 2:
Recovery skin is dry and peeling — it looks worse cosmetically than it feels. State 2 flare skin is red, hot, and the child is actively distressed. If the child is scratching as intensely as before, treat as State 2.
Photo references:
DermNet NZ — Pigmentation disorders (post-inflammatory pigmentation)
DermNet NZ — Atopic dermatitis subacute/chronic
Representative image — desquamation / flaking during skin recovery:
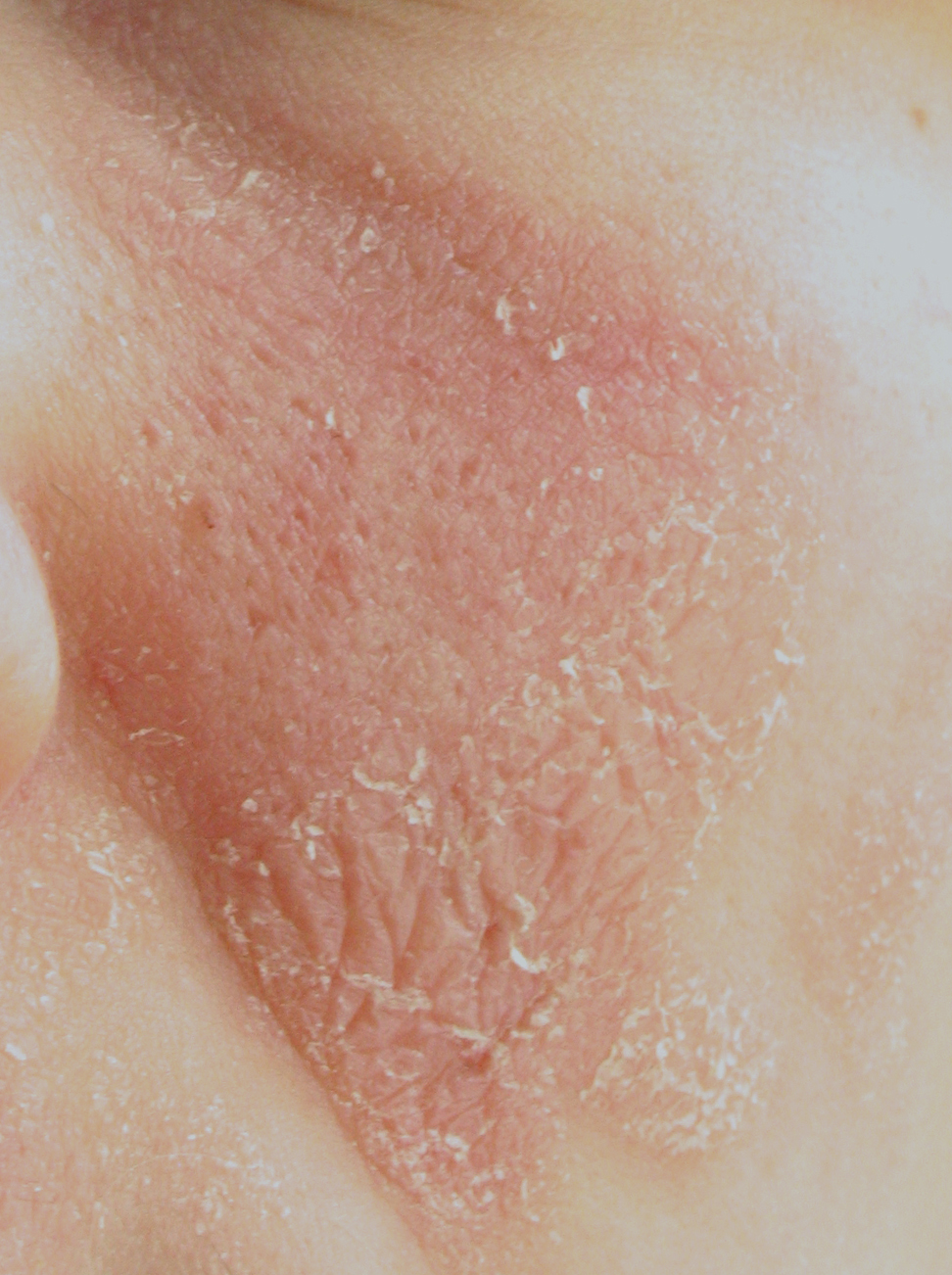
Pitke, CC BY 3.0, via Wikimedia Commons — source
This image shows the dry flaking/peeling appearance that recovering inflamed skin produces. The same type of desquamation is seen after eczema flares resolve.
Side-by-side comparison: eczema flare vs. infected eczema¶
| Feature | Active eczema (Phase 2) | Infected eczema (Phase 3) |
|---|---|---|
| Crust colour | White/grey (scratch scab) | Yellow/honey — key sign |
| Surface texture | Dry papules, rough | Wet, oozing, or waxy crust |
| Smell | Minimal | Noticeable sweet/sour odour |
| Pustules | Absent | Often present |
| Progression | Gradual worsening | Sudden worsening |
| Fever | Not typical | Possible (not required) |
| Responds to TCS alone | Usually yes within days | No — or worsens |
| What to add | TCS (Anticort/Advantan) | Octenisan + Bactroban; oral antibiotic only if infection is widespread/severe or child is unwell |
Treatment plan using available products¶
Phase 1 — Daily maintenance (between flares)¶
Goal: keep the skin barrier intact and reduce colonization risk.
- Bathe with Lipikar Syndet AP+ (or Exomega gel) — lukewarm, 5–10 min
- Pat dry gently
- Apply Lipikar Baume AP+M or Atoderm Intensive Baume within minutes to all skin
- Use XeraCalm A.D. cream for face if needed (lighter texture)
- If on a proactive maintenance protocol (agreed with clinician): apply Anticort to previous flare sites 2–3 times per week, even when skin looks calm
Phase 2 — Active flare (no sign of infection)¶
Goal: bring inflammation under control quickly.
- Continue Phase 1 routine
- Add Anticort once or twice daily to face/neck/fold flare areas (up to 14 days)
- Add Advantan once daily to body flare areas (not face; up to 14 days per site)
- Apply emollient over and around treated areas (consider Wet Wrap Therapy for severe flares: apply damp tubular bandages over heavy emollients/TCS to deeply hydrate and cool the skin, aiding penetration and sleep)
- Once controlled, step down to proactive maintenance
Phase 3 — Suspected infection or heavy Staph colonization¶
Signs: honey-coloured crusting, pustules, weeping, worsening despite TCS, odour.
- Replace regular cleanser with Octenisan wash lotion for the duration of the course (1–2 weeks). Alternatively, discuss adding dilute bleach baths (sodium hypochlorite, e.g., ~1/2 cup of 6% plain bleach per full bathtub, 2–3 times a week) as per standard AAD guidelines for recurrently infected eczema.
- Apply Bactroban cream to clearly infected patches 2–3x daily as prescribed (first choice); Xylanal gel as alternative if Bactroban is not available
- Apply emollient normally after washing
- Continue or restart TCS for the underlying eczema as directed
- If infection looks widespread, if there is spreading redness/cellulitis, or if the child has fever or seems unwell, seek medical review promptly because an oral antibiotic may be needed
- If there is no improvement within 48–72 hours, or if these episodes keep recurring, ask for review of the diagnosis, whether a skin swab is needed, and whether a decolonization plan is appropriate
Phase 4 — Recovery after a flare¶
Goal: support healing and restore barrier.
- Apply Cicabio Creme to fissured, excoriated, or healing areas
- Return to standard emollient (Lipikar Baume or Atoderm Baume) for broader skin
- Restart proactive maintenance protocol if not already in place
Gaps and recommendations¶
Critical gap — discuss with clinician¶
| Missing product | Why it matters | What to ask |
|---|---|---|
| Protopic 0.03% ointment (tacrolimus) or Elidel 1% cream (pimecrolimus) | The child is ~5 years old (≥2 years = approved age). A calcineurin inhibitor is the standard steroid-sparing option for face, eyelids, neck, folds, and proactive maintenance. Not having one means the available flare tool for sensitive areas is limited to mild hydrocortisone only. | Ask dermatologist/paediatrician to prescribe Protopic 0.03% for face/fold maintenance and flares; supported by NICE CG57 and EuroGuiDerm 2024 |
| Clear plan for antihistamine use | Xozal is now available, but oral antihistamines are not routine eczema treatment. The practical gap is knowing exactly when levocetirizine is worth trying, and when a short sedating option is more appropriate for a flare with major sleep disruption. | Ask clinician when to use Xozal (levocetirizine) for this child, what response would count as success, when to stop, and whether a short sedating antihistamine plan is needed for severe sleep-disrupting flares |
| Clear plan for recurrent infected eczema / oral antibiotics | The child has had multiple systemic antibiotic courses in different periods. Repeated antibiotic exposure can mean true recurrent bacterial infection, concurrent non-skin infections, resistance pressure, or a diagnostic mix-up. | Ask when to choose topical vs oral antibiotics, when to send a skin swab, whether nasal/skin decolonization should be used, and when repeated "infected eczema" should trigger a review for contact dermatitis, scabies, fungal infection, or another diagnosis |
Advanced therapies and escalations (for reference)¶
| Suggested therapy | Rationale |
|---|---|
| Dupilumab (Dupixent) | A biologic medication approved for children ≥ 6 months with moderate-to-severe eczema not adequately controlled by topical therapies. This is the main clinical next step if topical management fails. |
| Crisaborole 2% (Eucrisa) | A topical PDE4 inhibitor approved for mild-to-moderate eczema in children ≥ 3 months. An alternative non-steroidal option to calcineurin inhibitors, though it may cause transient stinging upon application. |
Useful additions (lower priority)¶
| Suggested product | Rationale |
|---|---|
| Plain white petrolatum (Vaseline) | Cheapest and very effective emollient for periods of intense dryness or between product stocks; excellent barrier; no risk of sensitisation |
| Hypochlorous acid spray (e.g., Poseidon Skin or similar) | Alternative to bleach baths for Staph colonization management; convenient spray-on format; useful if Octenisan washes are not enough |
Products with restricted use (do not use routinely)¶
| Product | Restriction |
|---|---|
| Betadine | Do not apply to eczema skin, inflamed areas, or post-flare skin. Reserve for isolated wound cleaning only. |
| Advantan | Not for face, eyelids, or folds. Body only. Maximum ~14 days per course. Do not use without current clinician guidance. |
| Ceclor / Amoxil / Augmentin | Do not restart or reuse as "eczema antibiotics" without clinician review. They are episode-specific systemic antibiotics, not routine flare medicines, and repeated courses increase resistance pressure and side-effect burden. |
| Xozal | Not routine eczema therapy. Use only as an adjunct when severe itch, urticaria-like symptoms, or a clinician-directed plan makes it reasonable; watch for drowsiness/somnolence. |
| Xylanal | For infected skin only; first-line remains Bactroban; Xylanal contains parabens — watch for contact sensitization. |
| Bactroban nasal | Only if part of an explicitly prescribed decolonization protocol. Not a routine eczema treatment. |
| MeliMpampa Κεραλοιφή (Σπαθόχορτο & Πρόπολη) | Not an evidence-based eczema treatment. Propolis is a contact allergen — elevated risk on atopic skin. Never use during active flares, infection, or on broken skin. Recovery skin only, spot-test first. |